Your Achilles’ Heel Isn’t Just a Myth: Understanding Achilles Tendinopathy
Understanding, Managing & Recovering
14 July 2025
What is the Achilles Tendon?
The Achilles tendon is the largest and strongest tendon in the human body. Located at the back of the lower leg, just above the heel, it connects the calf muscles — the gastrocnemius and soleus — to the heel bone (calcaneus). This powerful tendon plays a key role in everyday movement, helping you rise up onto your tiptoes, walk, run, and perform many sporting activities. In short, it's essential for nearly every step you take.
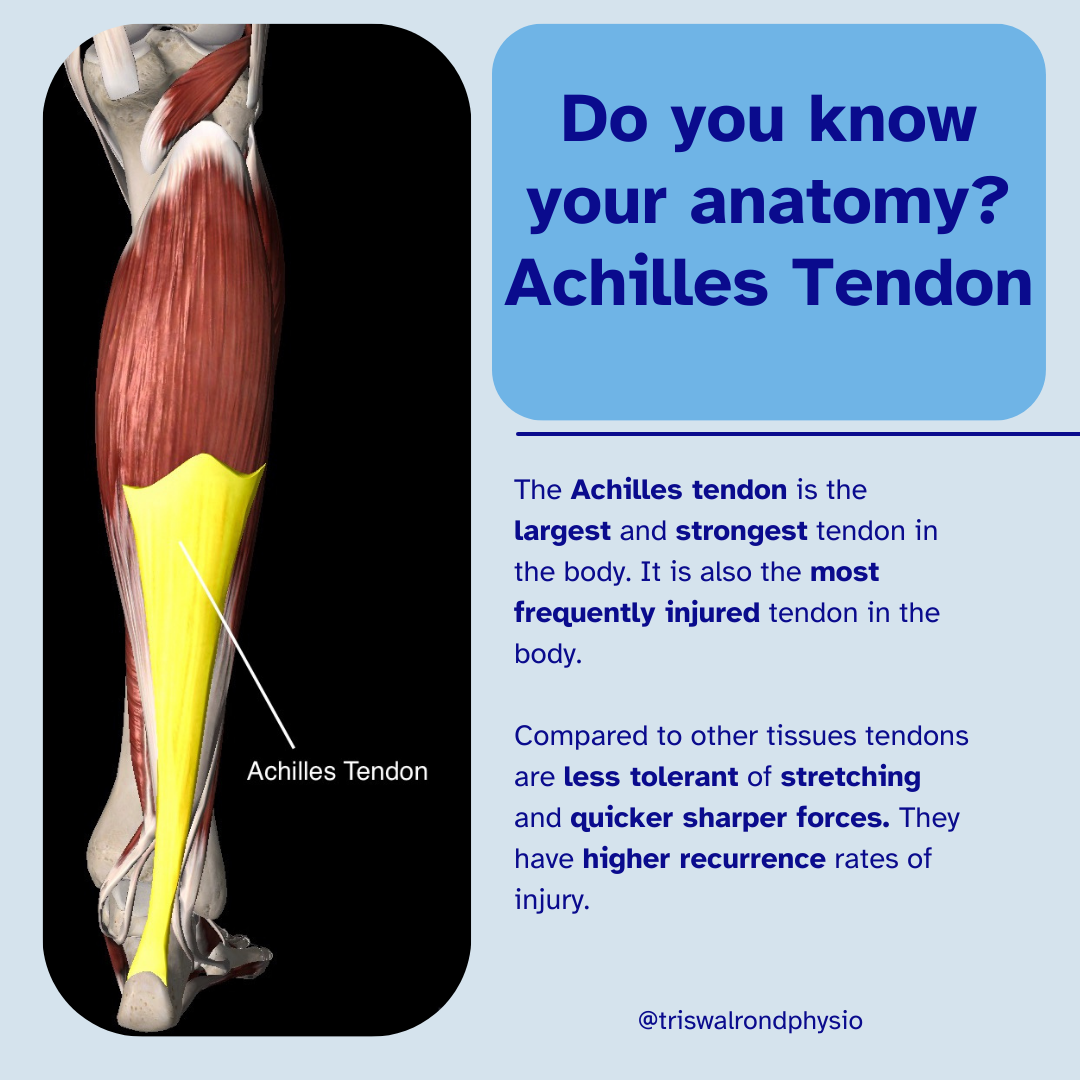
A unique aspect of the Achilles tendon is that part of it has a relatively poor blood supply, specifically the section about 2 to 6 cm above where it attaches to the heel bone. Because this “avascular zone” doesn’t receive as much circulation, it’s more prone to wear, tear, and degenerative changes over time.
Interestingly, people with Achilles tendon pain will often point right to this spot when describing their symptoms. For physiotherapists, this can be a valuable clue in identifying mid-portion Achilles tendinopathy.
What is Achilles Tendinopathy?
While the exact cause of Achilles tendinopathy isn't fully understood, one thing is clear — it typically develops when the tendon is overloaded. This excessive strain can outpace the tendon’s ability to adapt, leading to tiny (micro) tears in the tendon fibres. In response, the body attempts to repair the damage, which can result in ongoing inflammation, stiffness, and pain.
What Causes Achilles Tendinopathy?
Achilles tendinopathy can develop for a variety of reasons — and it’s not just about overtraining. Several factors can increase the strain placed on the tendon, raising the risk of injury. These risk factors include both lifestyle and physical elements:
Age: The condition is most common in people over 30, particularly men.
Weight: Carrying excess weight places more stress on the tendon.
Diabetes: Individuals with diabetes are at higher risk of developing tendon issues.
Stiff ankle joints: Limited mobility can alter movement patterns and increase strain.
Tight or weak calf muscles: Poor muscle flexibility or strength reduces the tendon’s ability to absorb force effectively.
Sudden increases in activity: A quick jump in walking, running, or sporting activity can overload the tendon.
Training errors: Common mistakes include increasing running distance too quickly, lack of variation in workouts, and adding hill running too soon.
Understanding and addressing these risk factors can help prevent Achilles tendinopathy or reduce its severity.
What are the Symptoms of Achilles Tendinopathy.
Pain just above your heel: Most people find that their pain is on the Achilles tendon, which can be tender to touch or if gently squeezed. Occasionally there is a visible lump or swelling in the painful region.
Pain after activity: most people will notice that their pain increases after a long walk/run or at the end of the day, particularly when they ‘relax.’ Some people can exercise through the pain but notice as time goes on the pain increases during activity and can prevent them from doing their normal exercise or sport.
Morning stiffness: Frequently people complain of stiffness around the Achilles in the morning, which usually eases after a few minutes of walking, but can take longer.
Physiology: Understanding Healthy Tendons vs Tendon Pathology
Tendons are made mostly of type I collagen, arranged in strong, parallel fibres designed to cope with high tensile loads. These fibres are maintained by specialised tendon cells called tenocytes, which constantly repair and remodel the tendon’s structure.
In a healthy tendon, there is a steady balance between collagen being broken down and new collagen being produced. Tendinopathy disrupts this balance. Instead of orderly fibres, the tendon begins to show microtears, collagen disorganisation, and the development of new, often fragile blood vessels (neovascularisation).
It’s important to remember that tendinopathy is not a classic inflammatory condition. Rather, it represents degenerative change within the tendon. This distinction matters: while anti-inflammatory treatments like corticosteroid injections may provide short-term relief, they can actually worsen tendon degeneration over time. Helping patients understand this often improves adherence to the slow and steady nature of tendon rehabilitation.
Classification of Achilles Tendinopathy
Achilles tendinopathy generally falls into two main categories, each with different clinical features and management considerations.
1. Mid-Portion Achilles Tendinopathy
This is the most common form, affecting the area roughly 2–6 cm above the heel bone (calcaneus). Key features include:
Diffuse thickening and tenderness through the midsection of the tendon
Stiffness first thing in the morning
Pain that often eases with gentle movement
Mid-portion tendinopathy responds particularly well to eccentric loading programmes, which help reorganise collagen and strengthen the affected tissue.
2. Insertional Achilles Tendinopathy
Insertional tendinopathy affects the point where the tendon attaches directly into the calcaneus. Typical findings include:
Pain localised right at the tendon insertion
Calcific changes or associated retrocalcaneal bursitis
Symptoms that worsen with activities involving deep dorsiflexion, such as uphill running or climbing stairs
Individuals with this type often do not tolerate traditional eccentric heel drops from a step because the increased compression at the insertion can aggravate symptoms. Modified exercises, such as heel raises performed on level ground without dropping the heel below neutral are usually more appropriate.
Self‑Help and Initial Management
Load modification - When dealing with Achilles tendon issues, managing your activity levels known as “optimal load” is key to recovery. Reducing stress on the tendon by temporarily cutting back on certain exercises and daily activities can help prevent further irritation. It's important not to do too much, too soon. Instead, gradually reintroduce activity over time as your symptoms improve. For the best results, work with your physiotherapist to determine the right balance of rest and movement tailored to your specific needs. The cornerstone of Achilles tendinopathy management lies in load modification and progressive loading. Although rest may temporarily relieve symptoms, complete unloading often results in tendon deconditioning and delayed recovery.
Footwear adjustments – use supportive shoes, heel lifts or insoles to reduce tendon stress
Simple pain relief – Simple pain relievers, such as paracetamol, can help manage discomfort associated with Achilles tendon issues. However, it's important to consult with a pharmacist or your healthcare provider to ensure these medications are safe and appropriate for you. Pain during exercise (up to ~4/10) is acceptable and expected, but sharp or excessive pain signals the need to regress or modify reps
Weight management & lifestyle – losing excess weight and improving overall activity reduces tendon load and promotes healing
Additional Physiotherapy Tools
Manual therapy: calf and ankle mobilisation, soft‑tissue massage to improve circulation and flexibility
Orthotics & heel wedges: support and help off-load the tendon.
Shockwave therapy (ESWT): a useful second-line, non-invasive option for chronic cases
Advanced options (for persistent or non-responding cases): PRP injections, ultrasound-guided tenotomy or scraping, and—rarely—surgery.

How Long Will Recovery Take?
Unfortunately, there’s no simple answer to how long it will take to recover from Achilles tendon issues. Tendon healing is a slow process by nature, and there are no quick fixes. Successful recovery often depends on consistent, active participation in your rehabilitation plan. Conservative (non-surgical) management has been shown to be the most effective approach for most people. However, if your symptoms haven't improved within 6 to 9 months, it's important to revisit your options with your physiotherapist and explore alternative treatments.
Final Thoughts
Achilles tendinopathy can be a frustrating and persistent condition, but with the right approach, recovery is absolutely possible. Managing your load, staying consistent with your rehabilitation exercises, and seeking guidance from a physiotherapist are key steps toward long-term improvement.
Remember, healing takes time—especially with tendons—but every small step counts. If you're struggling with Achilles pain or unsure about your treatment plan, don’t hesitate to reach out to a qualified physiotherapist. With the right support and a tailored program, you can get back to doing the things you love—stronger and more resilient than before.
Book an appointment today to take the first step toward recovery.