
Running and Arthritis: Should You Keep Running if You Have Knee or Hip OA?
Many runners with osteoarthritis (OA) wonder: “Will continuing to run make my arthritis worse?” Or “Should I stop running to protect my joints?” The good news is that current research offers some reassuring answers.
12 January 2026
Running Does Not Appear to Worsen Arthritis
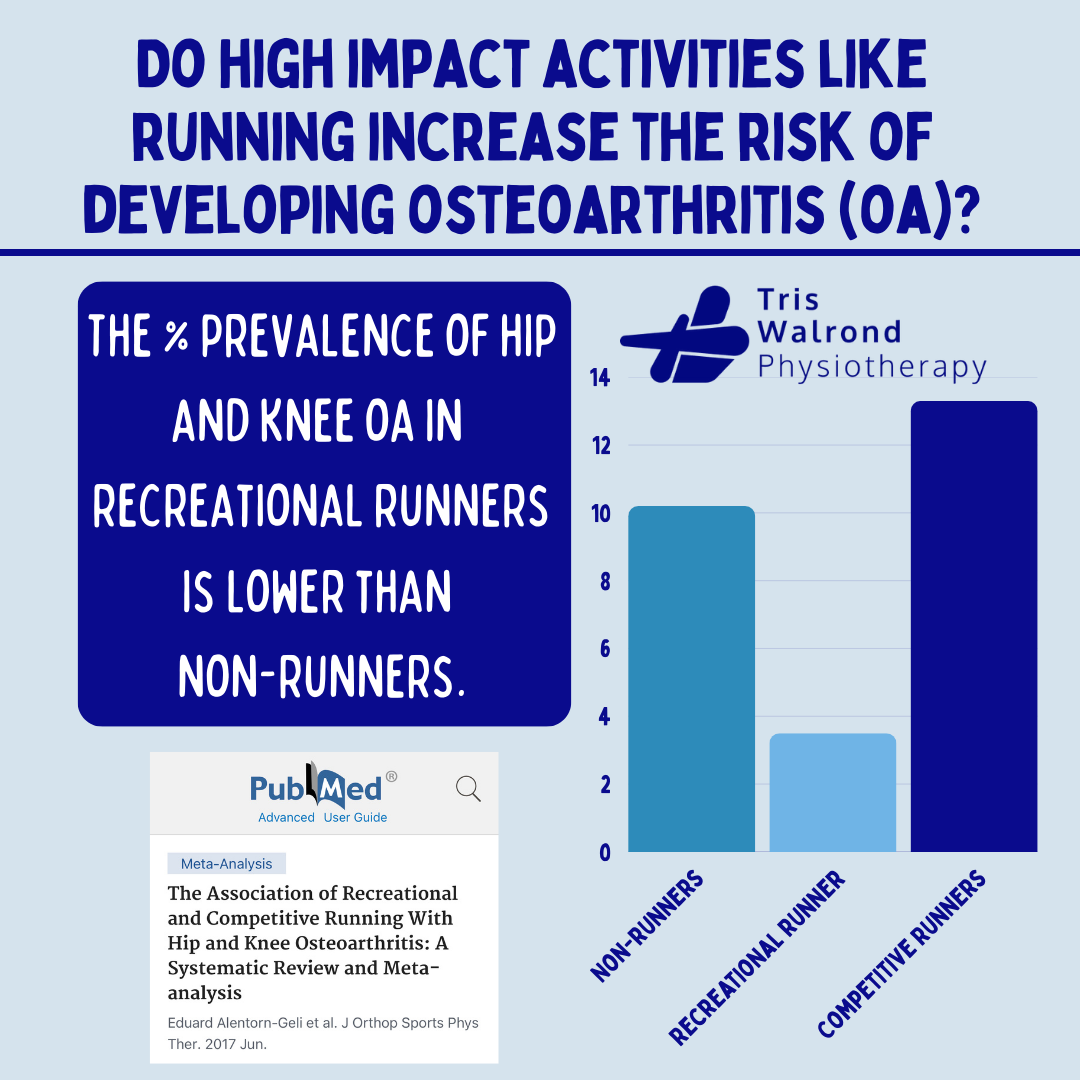
Longitudinal studies and systematic reviews consistently show that recreational running does not increase the risk of developing Osteoarthritis (OA), nor does it accelerate disease progression in people who already have knee or hip arthritis.

A 9-year longitudinal study (Lane et al., 1998) followed older adults with and without arthritis and found that runners did not have more progression of hip or knee OA than non-runners.
Data from the Osteoarthritis Initiative showed that running in individuals with existing knee OA did not increase pain or joint structural damage. In fact, some runners reported improved knee pain and better functional scores compared with those who did not run.

Takeaway: For most people, continuing to run is safe for joint health.
Recreational Running May Even Improve Symptoms
Interestingly, some individuals with OA who continue running experience less pain and better function than non-runners. How might this happen?

Improved muscle strength: Stronger muscles help support the joint and reduce stress on cartilage.
Joint nutrition: Moderate loading helps cartilage maintain healthy nutrition.
Cardiovascular and pain-modulation effects: Running stimulates endorphins and improves overall fitness, which can reduce the perception of pain.
Important caveat: Symptom improvement is not guaranteed for everyone. Load tolerance, injury history, and running technique all influence outcomes.
Precautions: High-Volume and Elite Running
While recreational running appears safe, research shows that elite or competitive runners with very high training volumes may have higher OA prevalence, particularly when weekly mileage exceeds 90 km per week.

Factors likely contributing to this increased risk:
High cumulative joint load over years
Increased injury exposure
Limited recovery time between intense training sessions
Key point: This finding does not mean running causes OA, but it highlights that extreme loads over time may contribute to joint stress. Recreational runners rarely reach these volumes.
Practical Advice for Runners with OA
If you have arthritis, the goal isn’t to stop running, it’s to run smart. Here are some tips:
Listen to your body: Mild flare-ups are normal, but persistent pain deserves attention.
Manage load: Gradually increase mileage or intensity; avoid sudden spikes.
Strength training: Support joints with hip, quadriceps, hamstring, calf and core exercises.
Recovery: Rest and cross-training help reduce cumulative stress.
Seek professional guidance: A physiotherapist can individualise your plan.
Bottom Line
Recreational running does not worsen hip or knee arthritis.
Some runners with OA may experience improved pain and function.
High-volume, elite-level running carries higher prevalence, but this is rare for recreational athletes.
Running is generally joint-safe and potentially joint-protective when you respect your limits, manage load, and incorporate recovery and strength training.

Arthritis does not automatically mean “stop running.” Recreational running does not worsen hip or knee arthritis, and some runners may even see improved pain and function. If you’re unsure how to run safely with OA, booking a physiotherapy session can help tailor your training, manage load, and prevent flare-ups.