
Understanding and Managing Low Back Pain: What You Need to Know
Learn what’s behind your back pain—and what you can do about it.
4 November 2025
Understanding and Managing Low Back Pain: What You Need to Know
Low back pain is one of the most common reasons people seek medical care, affecting up to 80% of adults at some point in their lives. It can range from a dull ache to sharp, debilitating pain and can significantly interfere with daily activities. Understanding its causes, risk factors, and treatment options is key to effective management and prevention.
Low back pain can be alarming, especially during a flare-up. Even a minor strain can trigger thoughts of serious damage. However, the truth is that most back pain is not caused by serious disease or pathology, and serious or permanent damage is rare.
In this post, we’ll break down the facts about back pain, common myths, what red flags to watch for, and how you can actively manage your symptoms to get back to living your life.
The Truth About Low Back Pain
Low back pain is incredibly common, and in most cases, it improves within a few days to weeks. Even if some discomfort lingers, it doesn’t usually mean something serious is wrong.
✅ The spine is strong. It’s built for movement. ❌ Prolonged rest is not helpful. Staying still for too long can actually slow your recovery.
Why Movement Matters
One of the most important things you can do is keep moving. Movement helps:
Reduce stiffness
Maintain strength
Boost circulation and healing
Prevent deconditioning and mood-related setbacks
People who stay active during episodes of back pain tend to recover faster and cope better in the long term.

When to seek urgent help: Red flags
While most cases of back pain improve with conservative management and physiotherapy, there are certain symptoms that should never be ignored. Some signs may indicate a serious underlying condition that requires urgent medical intervention. One such condition is Cauda Equina Syndrome - a rare but serious spinal emergency that can lead to permanent nerve damage if not treated promptly.

Cauda Equina Syndrome (Seek emergency care immediately if you notice):
Loss of sensation or pins and needles in the inner thighs or genital area (commonly described as “saddle anaesthesia”)
Numbness in or around the anus or buttocks
A change in the ability to feel toilet paper when wiping
Increasing difficulty starting or stopping urination
Loss of bladder sensation or control
Urinary leakage or a recent need to use pads
Not knowing when the bladder is full or empty
Inability to control bowel movements or unexpected leakage
Loss of sensation during bowel movements
New difficulties in achieving an erection or ejaculation
Decreased genital sensation during sexual activity


These symptoms may point to compression of the nerves at the base of the spine and should never be ignored.
Other signs that need urgent medical review:
Back pain accompanied by fever
A pulsating sensation in the abdomen
Pain after a fall or trauma
Sudden, unexplained weight loss
New back pain if you're over 55 or have a history of cancer, steroid use, osteoporosis, or substance use

So, What Causes Most Back Pain?
Most cases of low back pain are caused by muscles, ligaments, joints, or poor movement patterns. Common contributing factors include:
Poor sustained postures over time
Muscle weakness or stiffness
Lack of flexibility or movement
Stress, anxiety, or fatigue
💡 Tip: “Slipped discs” and “trapped nerves” are much less common than people think, and often heal without surgery.
A Modern Approach: The Biopsychosocial Model
We now understand that pain is influenced by more than just physical issues. Factors that can impact your pain include:
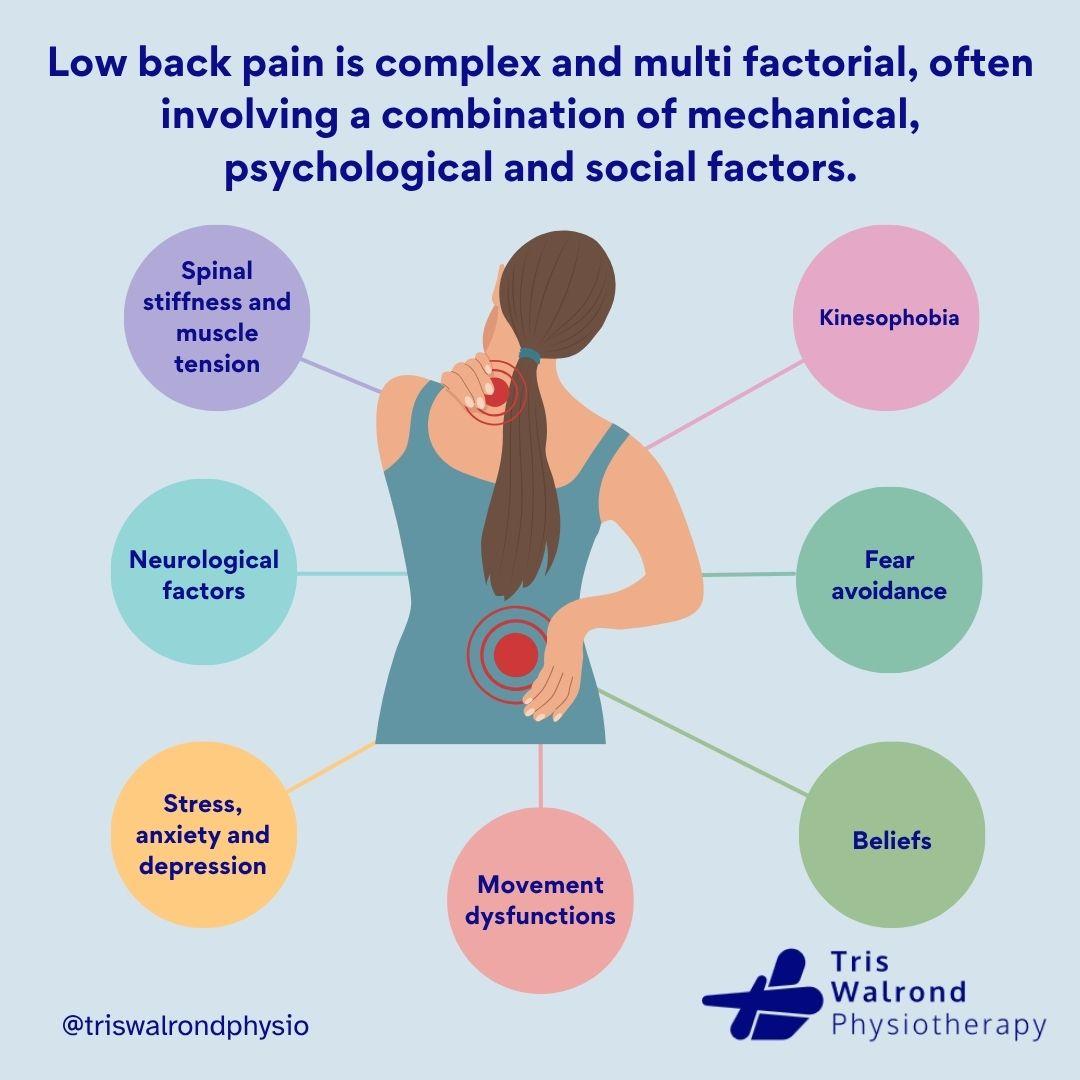
🧠 Psychological:
Stress and anxiety
Depression or low mood
Catastrophic thinking
👥 Social:
Work stress
Lack of support
Sleep disturbance
🏃 Biological:
Poor fitness
Previous injuries
Health conditions
Contributing Lifestyle Factors
Cardiovascular fitness: Low activity levels are linked to more back pain.
Emotional wellbeing: Mood and pain are closely related. Managing stress can reduce symptoms.
Sleep: Poor sleep worsens pain. Prioritise good sleep habits.
Strength & flexibility: Whole-body strength and mobility support spinal health.
Weight: There is a strong association between being overweight and low back pain. Excess weight can increase the physical demand on the body and contribute towards low grade inflammation.
Smoking: Smoking increases the risk of developing over 50 serious health conditions including cancer, heart disease and stroke. Research has also identified smoking has an association with low back pain.
Posture and Positioning: The Myths
There is no perfect posture. Staying in one position for too long—not the position itself—is what contributes to discomfort.
💡 Tip: Change positions regularly and listen to what feels best for your body.
Do You Need a Scan?
In most cases: No.
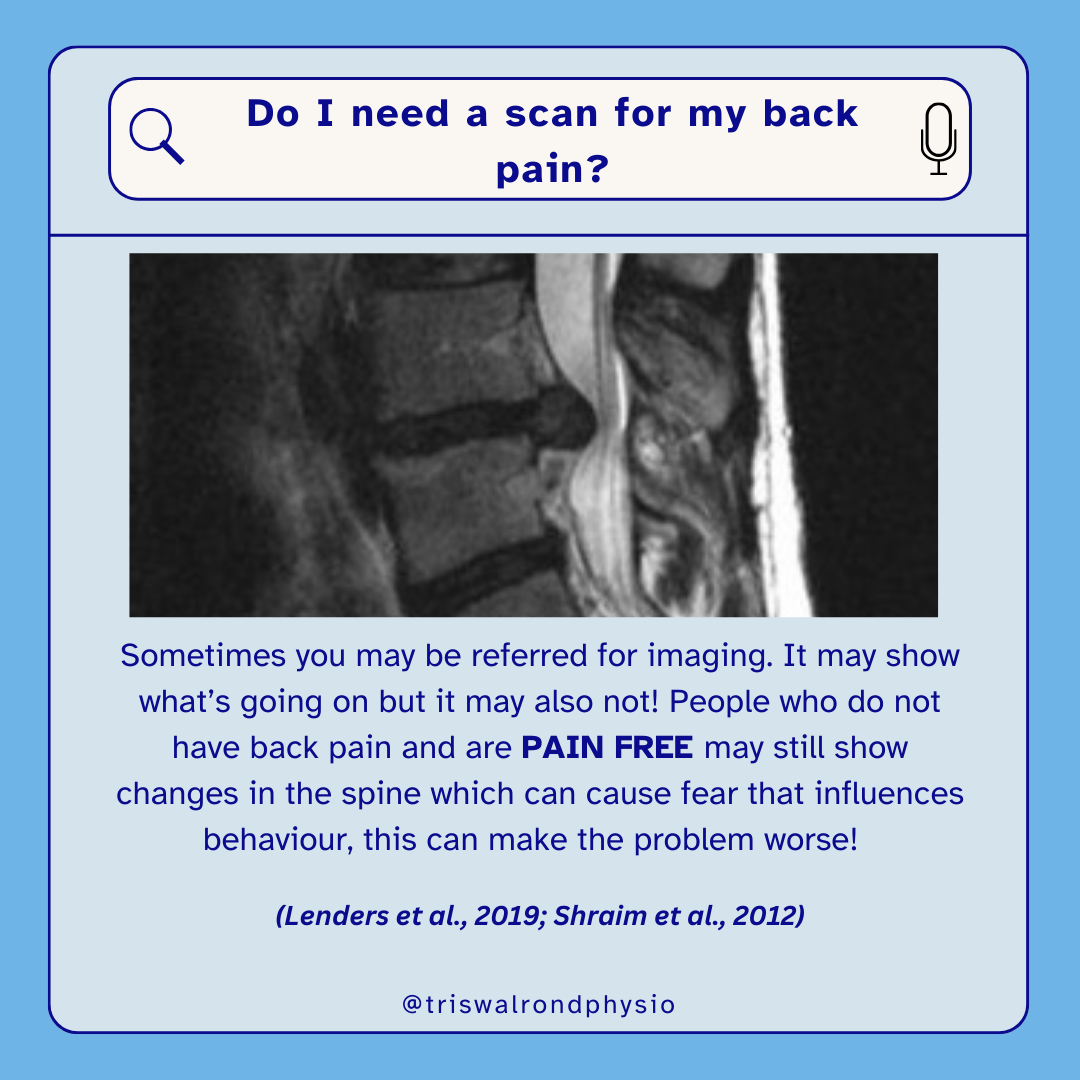
Why?
X-rays and MRIs rarely change treatment or improve outcomes.
MRI findings often don’t correlate with pain—many people with “abnormal” scans have no symptoms at all.
Scans can cause unnecessary worry and may delay recovery.
Scans are only recommended if:
Symptoms suggest a serious underlying condition
You’re being considered for surgery
There’s been a significant injury (e.g., fracture risk)
How to Manage Back Pain
✅ What Helps:
Keep active—movement is your medicine
Use pain relief if needed (paracetamol or ibuprofen, as advised by your GP)
Hot/cold therapy (ice in first 72 hrs, then heat)
Massage/manual therapy (as a supportive treatment)
Graded exercise programs (build slowly and steadily)
❌ What Doesn’t Work Alone:
Bed rest
Passive therapies without exercise
Alternative treatments without proven benefit (ultrasound, electrotherapy, etc.)
Understanding Flare-Ups
Flare-ups are normal. They don’t mean your back is "damaged again."
What to Do:
Don’t panic—stick with your routine as best as possible
Use pacing: break tasks into chunks, rest in between
Adjust activity, don’t stop entirely
Return to normal activity as soon as you can
Everyday Advice for a Healthy Back
SITTING: Choose a comfortable position, move often (every 30 to 45 minutes).
SLEEPING: A supportive mattress may help. Take pain relief before bed if needed. A pillow in between the thighs can help.
LIFTING: Bend your knees, keep the load close, avoid twisting.
DESK WORK: Adjust your setup for comfort. Take standing breaks.
DRIVING: Set up your seat well. Take movement breaks on long journeys.
SPORTS: Continue with modifications if needed. Swimming is excellent early on.
SEX: Keep going, adapt positions for comfort if needed.
The Role of Physiotherapy and Exercise
Research shows that graded exercise programs are the most effective way to manage and recover from low back pain.
Physiotherapy Can Help You:
Regain movement
Build strength and stability
Restore confidence in your body
Prevent recurrent episodes
Set long-term goals for healthy, active living 💡 Tip: You may feel some mild discomfort with exercise, that’s okay! As long as pain stays below a 3–4/10, it’s safe to keep going.
Education and Self-Management for Low Back Pain
Managing low back pain effectively starts with understanding it. Low back pain is common and often self-limiting, meaning it usually gets better on its own. Learning about the nature of back pain can help reduce fear and anxiety, which in turn can lessen pain and speed up recovery. Remember, movement is safe and important for healing.
Final Thoughts: What Now?
Back pain can feel overwhelming, but the key to recovery is staying active and gradually building back strength and function.
Simple Rules to Remember:
Keep moving - movement heals
Don’t fear pain - use it as a guide, not a stop sign
Adjust, don’t avoid
Set small, achievable goals
Plan for setbacks - flare-ups are normal
Stay consistent and stay positive
Need Help?
A physiotherapist can provide a personalised rehab plan that takes into account your unique goals, lifestyle, and symptoms.
Book a consultation today and start your journey back to full movement, confidence, and activity.
Reduce Pain. Increase Strength. Improve Function.